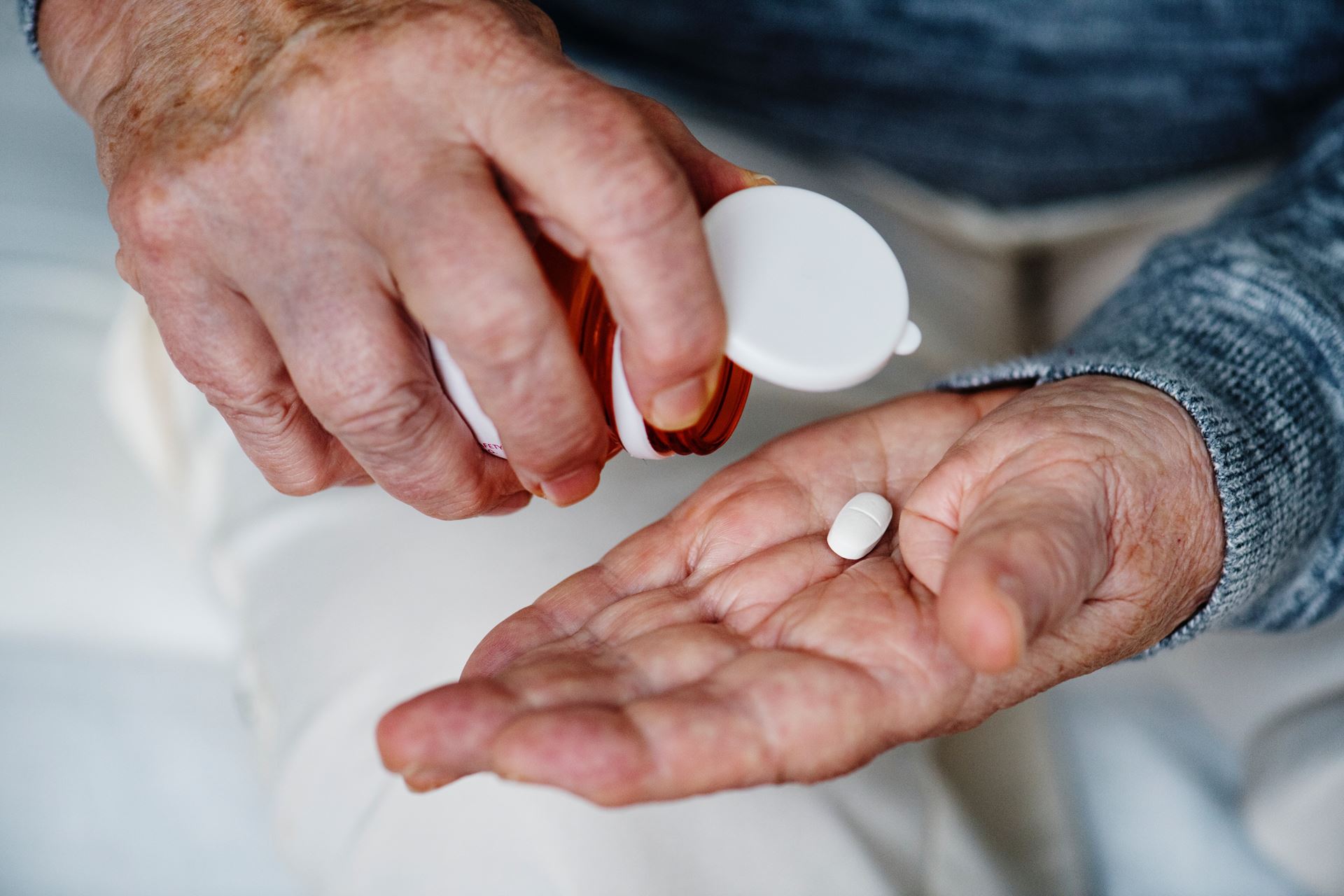
Welcome to Holmes Chapel Health Centre
‘Our aim is to provide the best possible health care for you and your family.’ Our practice is classified as semi-rural, based in a purpose built health centre in the heart of the community in Holmes Chapel.
We have a growing practice population, currently around 13,000 patients, served by an extended Primary Health Care Team including doctors, practice and community nurses, reception staff, physiotherapists and health visitors. We are part of the NHS Cheshire and Merseyside Integrated Care Board.
Mission Statement
To provide professional, accessible, high‑quality healthcare that patients and the community can trust.
Our Vision
- · Be a recognised centre for high‑quality teaching and training.
- · Deliver excellent patient outcomes in a safe, welcoming, and respectful environment.
- · Use technology effectively to enhance care, communication, and efficiency.
- · Work collaboratively with our rural community to provide accessible local services.
Our Values
Accountable
We take responsibility for our actions and are open and transparent with those who use our services.
Caring
We place our patients and local community at the centre of everything we do.
Fair
We treat everyone consistently and courteously, showing compassion and valuing each person as an individual.
Innovative
We use resources and technology to deliver the best service possible and continually improve.
Professional
We provide high‑quality medical care and respond to the needs of our community.
Online Services
NHS App and your NHS account
Download the NHS App, or open the NHS website in a web browser, to set up and log in to your NHS account. Owned and run by the NHS, your NHS account is a simple and secure way to access a range of NHS services online.
For more information click here
A34 Road Closure
RSV Fact Sheet publication
New guidance has been published regarding the RSV Vaccinations, please click on the link below to read more
Opening Times
Have Your Say
NHS Friends and Family
Page created: 27 September 2021